Some skin conditions can often seem like a guessing game. Itchiness here, redness there—could it be atopic dermatitis or perhaps psoriasis? And where exactly does eczema fit into the picture? Differentiating atopic dermatitis and psoriasis can be challenging when common symptoms like dry, inflamed skin seem to crisscross each disorder.
Don’t worry; you’re not alone in your quest for answers. That’s why we’ve turned to our trusted skin health expert, Dr. Ina-Andreea Mintas, a Dermatologist. Her extensive knowledge and comforting approach to patient care will help us understand the differences between eczema, atopic dermatitis, and psoriasis.
Find clarity amidst the confusion—because when it comes to your health, you deserve to be informed, secure, and confident in your understanding. Let’s arm you with some skin disorder know-how and care tips along the way.
First of all, what are these conditions?
Both atopic dermatitis and psoriasis are common, chronic inflammatory skin diseases.
Atopic dermatitis, a type of eczema, is a common skin disorder that usually starts in early childhood and can last into adulthood. Symptoms include itchy, red patches on the skin that are often scaly but sometimes develop into watering blisters. It’s not contagious and doesn’t cause long-term damage to the skin, however, it can be very annoying.
Psoriasis is an autoimmune condition that presents as a skin rash with itchy, scaly patches, most commonly appearing on the knees, elbows, trunk, and scalp. The manifestations of psoriasis vary widely in appearance by each person.
Skin rashes or patches can be different colors depending on the skin tone; on lighter skin, they will be pink or red.
These are two different skin disorders; atopic dermatitis can’t turn into psoriasis. But it is hard to tell them apart because they share similar symptoms.
How can we distinguish atopic dermatitis from psoriasis?
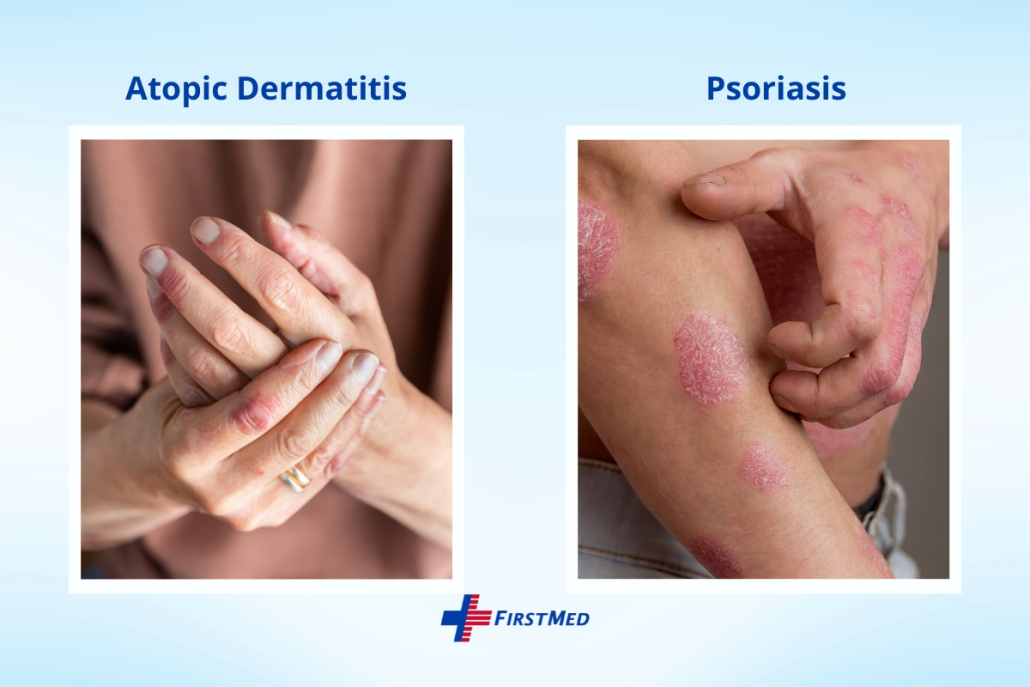
Although they look similar, there are some significant differences between them:
Primary symptoms of atopic dermatitis:
- Dry skin with itching involves an itch-scratch cycle: You itch, then scratch, causing a rash, which makes you itch more and scratch again.
- Rubbing causes increased inflammation and thickening of the skin, and heavy scratching may also cause an infection.
- Pustules (small pus-filled bumps) form on the skin surface, which may leak and crust over.
Typical symptoms of psoriasis:
- Dry, cracked skin that may bleed;
- Varied rash ranging from dandruff-like scaling spots to significant eruptions over the body;
- Itching, burning, or soreness may occur;
- It can also cause nail problems: yellowish discoloration and thickening of nails.
Flare-ups may last for a few weeks or months and then subside, but the duration can vary from person to person. If your symptoms are severe or persistent, you should see a dermatologist.
Now that we’ve outlined the symptoms, let’s dive deeper into the differences between atopic dermatitis and psoriasis.
What causes atopic dermatitis and psoriasis?
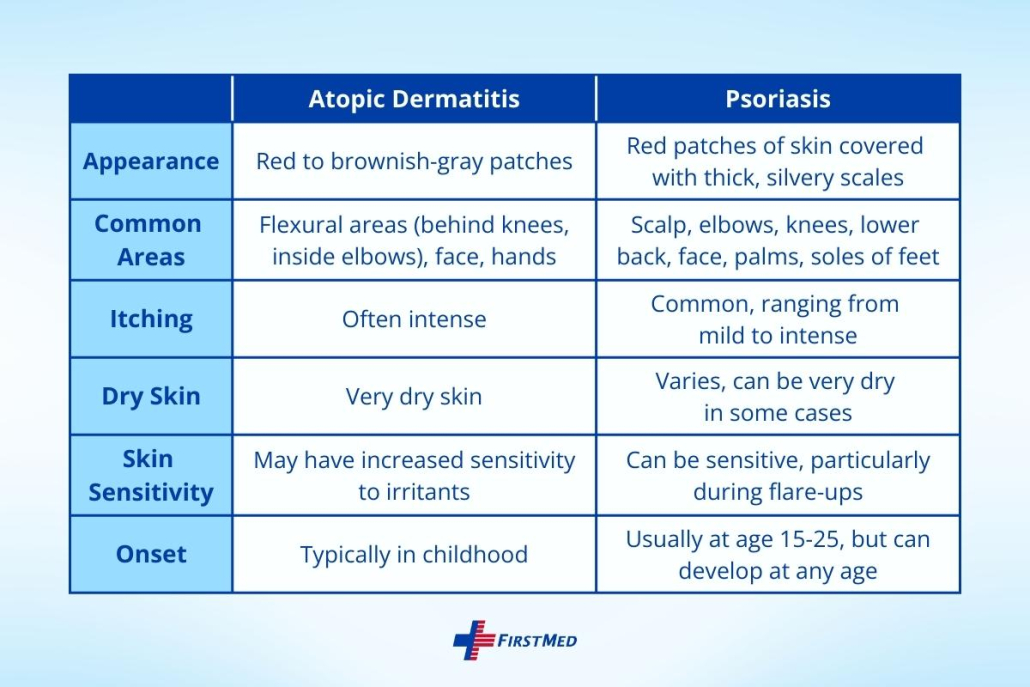
The exact cause of these conditions is unknown, but they’re thought to be due to a combination of genes, the environment, and immune system abnormalities.
- Both psoriasis and atopic dermatitis are typically triggered by dry (dehydrated) skin.
- Cold or dry weather can also dehydrate the skin, exacerbating itching in atopic dermatitis patients or triggering symptoms of psoriasis.
- Stress and anxiety may also lead to increased stress hormone production, which in turn causes skin redness, swelling, and irritation, which affects both conditions.
In addition to these factors, atopic dermatitis and psoriasis have unique triggers that are specific only to each of them:
Atopic dermatitis triggering factors
Though each person with atopic dermatitis experiences symptoms differently, some common factors can trigger flare-ups:
- Environmental allergens: Substances like pollen, pet dander, and dust mites can trigger a flare-up.
- Irritants: Common irritants include rough fabrics, soaps, detergents, and perfumes.
- Food allergies: Certain foods, such as eggs, milk, wheat, soy, and peanuts, can cause eczema and atopic dermatitis flare-ups in some people.
Psoriasis triggers
Psoriasis is a more complex condition, and its triggers are equally diverse:
- Infections: Conditions like strep throat can lead to guttate psoriasis, which appears as tiny red spots on the skin.
- Injury to the skin: Cuts, scrapes, bug bites, sunburns, and other skin injuries can trigger a psoriasis flare.
- Medications: Certain medicines, such as beta-blockers and lithium, can trigger or worsen psoriasis.
- Alcohol and smoking: Both these elements may worsen psoriasis and make treatments less effective.
Identifying and avoiding triggers is the best way to control your condition if you have atopic dermatitis or psoriasis. But remember, these factors can be different for each person. Something not listed here may still cause a flare-up in some people.
Common types of atopic dermatitis and psoriasis
Atopic dermatitis can take some specific forms, like
- Hand dermatitis, which is caused by chemical irritants in the environment or
- Erythroderma: a widespread reddening of the skin due to inflammation.
Psoriasis, on the other hand, has several types:
- Plaque psoriasis, for instance, can appear on different body parts with dry, itchy, raised patches covered in scales.
- Nail psoriasis affects fingernails and toenails, causing pitting, abnormal growth, and discoloration.
- Other types of psoriasis, such as guttate, inverse, pustular, and erythrodermic psoriasis, each have their unique manifestations and triggers.
Detection and treatment
Detection of both conditions primarily involves a physical exam by an experienced dermatologist. The specialist examines your skin closely and considers your personal and family history.
Can atopic dermatitis and psoriasis be cured?
The short answer is no, but you can manage both conditions. Atopic dermatitis and psoriasis are chronic, lifelong diseases that occasionally flare up. But with proper treatment and self-care, you can manage their symptoms and reduce their impact on your life. The most important thing is to avoid triggers, but there are some other things you can do to keep symptoms under control.
These practices can avoid flare-ups:
- Don’t scratch or rub (wear soft clothing).
- Reduce stress: try to relax as much as possible or practice mindfulness.
- Protect the skin from drying and rehydrate it as much as possible:
- Avoid hot water: shower quickly with lukewarm water or put some herbal oil in the water if you prefer bathing.
- Moisturize often using oily creams, which are suggested for dehydrated skin.
- Drink a lot of water and other fluids.
- The doctor may recommend topical corticosteroids that reduce swelling, redness, and itching during flare-ups.
Psoriasis symptoms usually can be treated with topical preparations and light therapy. In more severe cases, with extensive skin symptoms and arthritis, the doctor may suggest some medications.
In conclusion
Due to overlapping symptoms, differentiating atopic dermatitis from psoriasis can be challenging. Recognizing personal triggers and getting accurate diagnoses are essential to effectively managing these conditions.
Remember, your skin is unique, and treatments are not one-size-fits-all. Always consult a healthcare professional for personal advice, and FirstMed is here to guide you through your skin health journey.
Dr. Ina-Andreea Mintas, FirstMed’s Dermatologist
Edited by: Dorottya Fekete




